
Food Allergies & Intolerances in Children
A Practical Guide for Families
If your child reacts to certain foods, has ongoing tummy issues, eczema flare-ups, or unexplained symptoms, it can feel overwhelming trying to work out what’s normal — and what’s not.
As a paediatric dietitian on the Central Coast, we support families navigating food allergies, intolerances, elimination diets, and reintroductions in a safe and evidence-based way.
This guide explains the difference between allergies and intolerances, when testing is appropriate, and how to protect your child’s nutrition while managing food reactions.
Food Allergy vs Food Intolerance: What’s the Difference?
Although the terms are often used interchangeably, food allergies and food intolerances are very different.
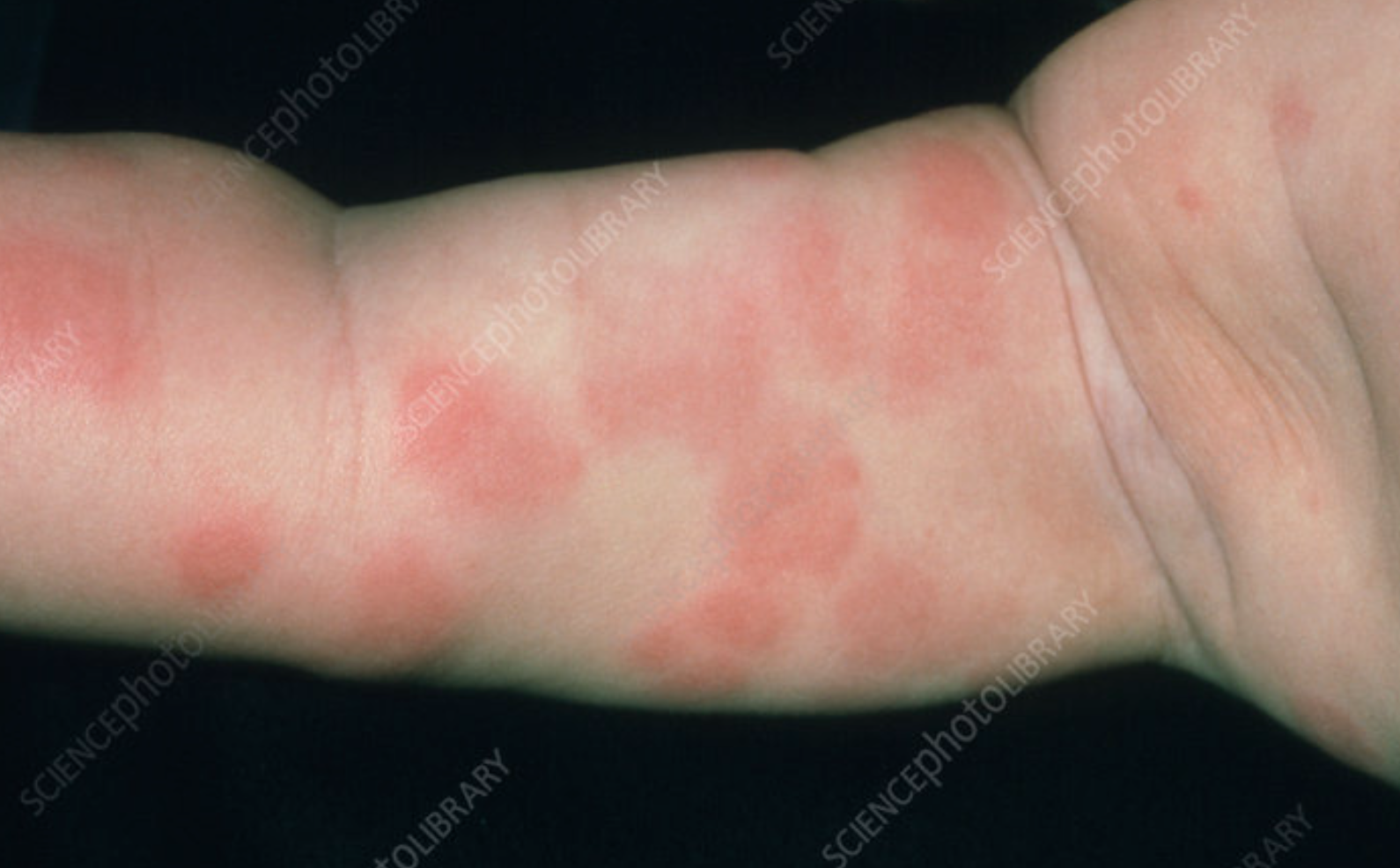
A food allergy involves the immune system. Symptoms may include hives, swelling, vomiting, wheezing, or in severe cases, anaphylaxis. These reactions are typically rapid and require medical assessment and diagnosis.
A food intolerance does not involve the immune system. Instead, it affects digestion and may cause bloating, diarrhoea, abdominal pain, reflux, or changes in bowel habits. Intolerances are often dose-dependent, meaning small amounts may be tolerated.
Understanding this distinction is important, as unnecessary long-term food restriction can impact growth and nutrient intake.
If you are unsure whether your child’s symptoms are affecting their growth or appetite, our Feeding & Growth Guide explains how nutrition and growth patterns are assessed together.

When Should You Test for Food Allergies?
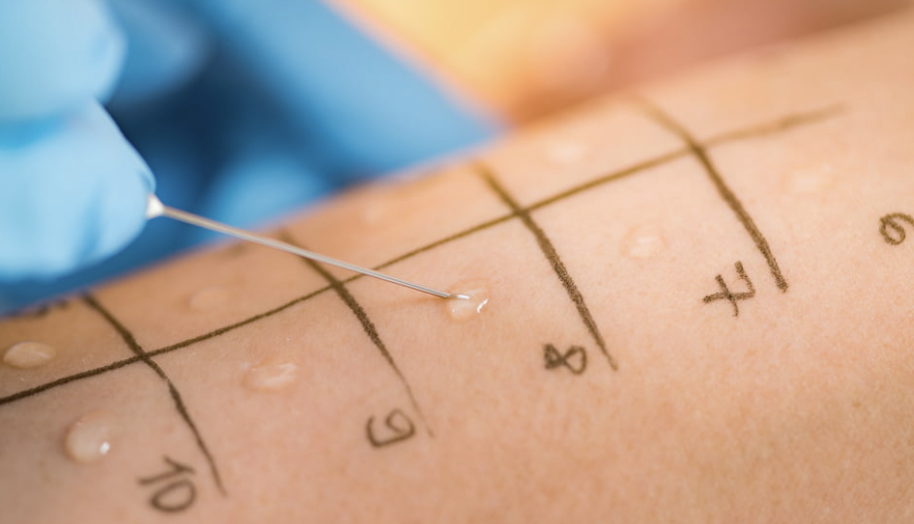
Testing should be guided by a GP or paediatrician based on a clear history of symptoms. Random or broad “food sensitivity” panels are often misleading and may result in unnecessary restriction.
If your child has experienced immediate reactions such as hives, swelling, or breathing changes, medical assessment is urgent. For more subtle gastrointestinal symptoms, a structured approach may be recommended before eliminating foods.
Working with a dietitian ensures that any elimination diet is nutritionally adequate and appropriately monitored.
Common Food Allergies in Australian Children
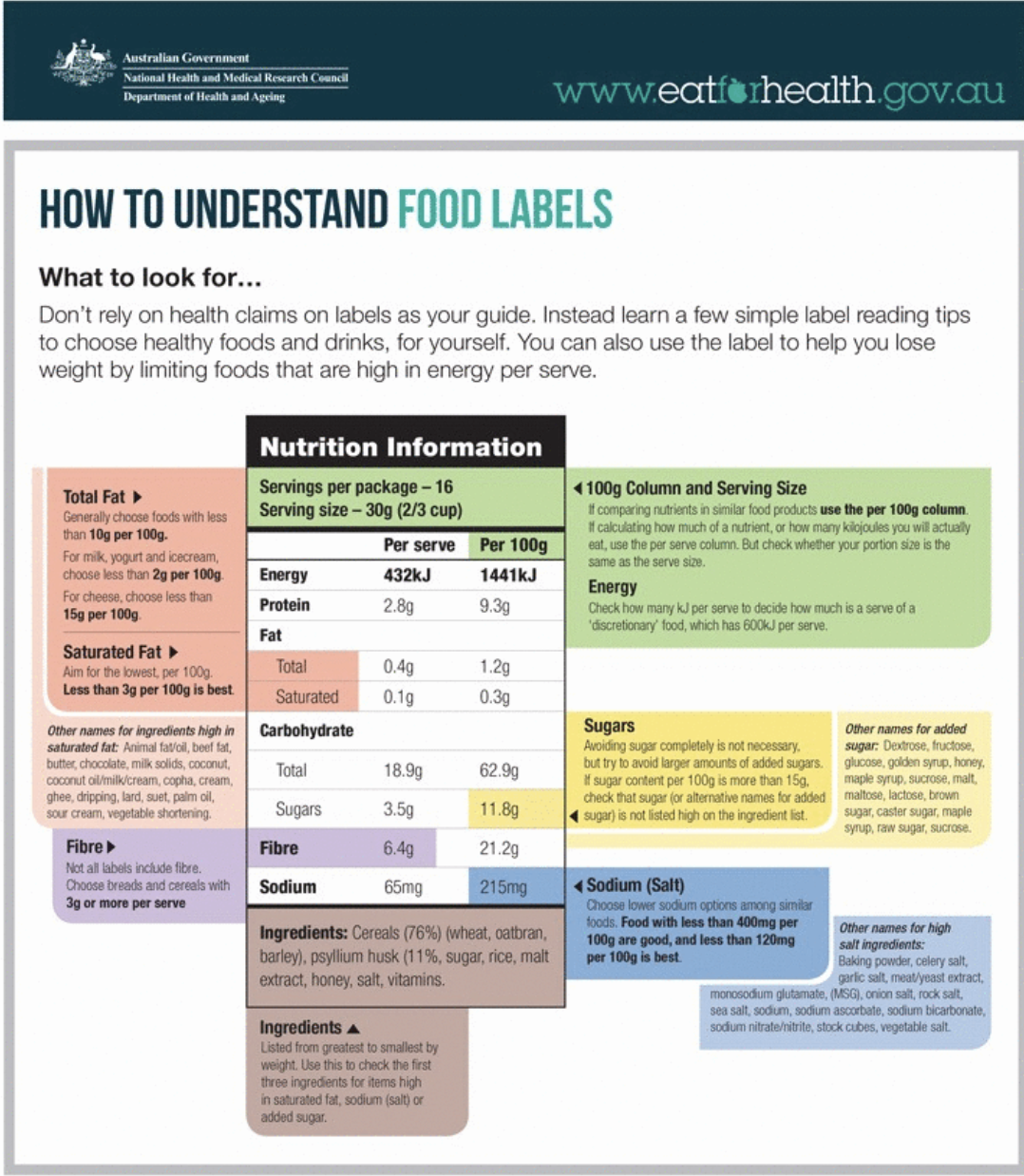
In Australia, common food allergens include cow’s milk, egg, peanut, tree nuts, soy, wheat, sesame, fish, and shellfish. Many children outgrow some allergies, particularly milk and egg, but proper medical guidance is essential before reintroducing foods.
For families on the Central Coast managing diagnosed allergies, everyday situations such as school lunches, birthday parties, and eating out can feel stressful. Careful label reading and practical planning help reduce anxiety while maintaining variety.
A paediatric dietitian can help ensure your child’s diet remains balanced even when major food groups are excluded.

Gastrointestinal Symptoms and Intolerances
Some children experience ongoing abdominal pain, constipation, diarrhoea, bloating, or reflux without confirmed allergies. In certain cases, short-term dietary strategies may be trialled under professional supervision.
It is important that restrictive diets, including low FODMAP approaches, are not implemented long-term without review. In growing children, overly restrictive diets can affect gut microbiome diversity and nutrient intake.
Children with multiple allergies or long-term dietary restrictions may be at increased risk of iron deficiency, low calcium intake, poor weight gain, or slowed growth.
Monitoring growth percentiles alongside dietary intake helps identify concerns early. Most children can thrive with allergies when supported appropriately.
Assessment looks at the whole picture: growth history, dietary patterns, symptom timing, stress factors, and medical history.
If you are concerned about your child’s weight, appetite, or nutrient intake, a paediatric dietitian assessment can provide clarity and reassurance.

Managing Elimination Diets Safely
Removing foods without guidance can sometimes create unintended nutrient gaps. For example, eliminating dairy without adequate alternatives may reduce calcium intake. Removing wheat may impact fibre and B-vitamin intake.
Children who are already selective eaters are particularly vulnerable to further restriction. If your child also struggles with limited variety, you may find our guide on Fussy Eating in Toddlers & Children helpful.
The goal of dietary management is not simply avoidance — it is safe substitution, nutritional adequacy, and, where appropriate, structured reintroduction.
You may benefit from paediatric nutrition support if you are searching for:
Paediatric dietitian Central Coast food allergy support
Child with suspected food intolerance
Dairy free child nutrition help
Managing multiple food allergies in children
Child not gaining weight due to restricted diet
Supporting healthy growth, development, and confidence.
With experience supporting people through complex medical conditions as well as the challenges of parenting and family life, Ellie helps families move away from stress and self-doubt toward clarity, confidence, and trust around food.
The aim is not perfect eating, but a positive relationship with food that supports your child’s growth, development, and wellbeing over time.
If you’re concerned about your child’s nutrition, feeding, or growth, you can book a paediatric dietetics appointment on the Central Coast with Ellie.


